Pathological analysis of the deposition of IL-6 in the central nervous tissues in Neuromyelitis Optica Spectrum Disorders
Abstract
Background:
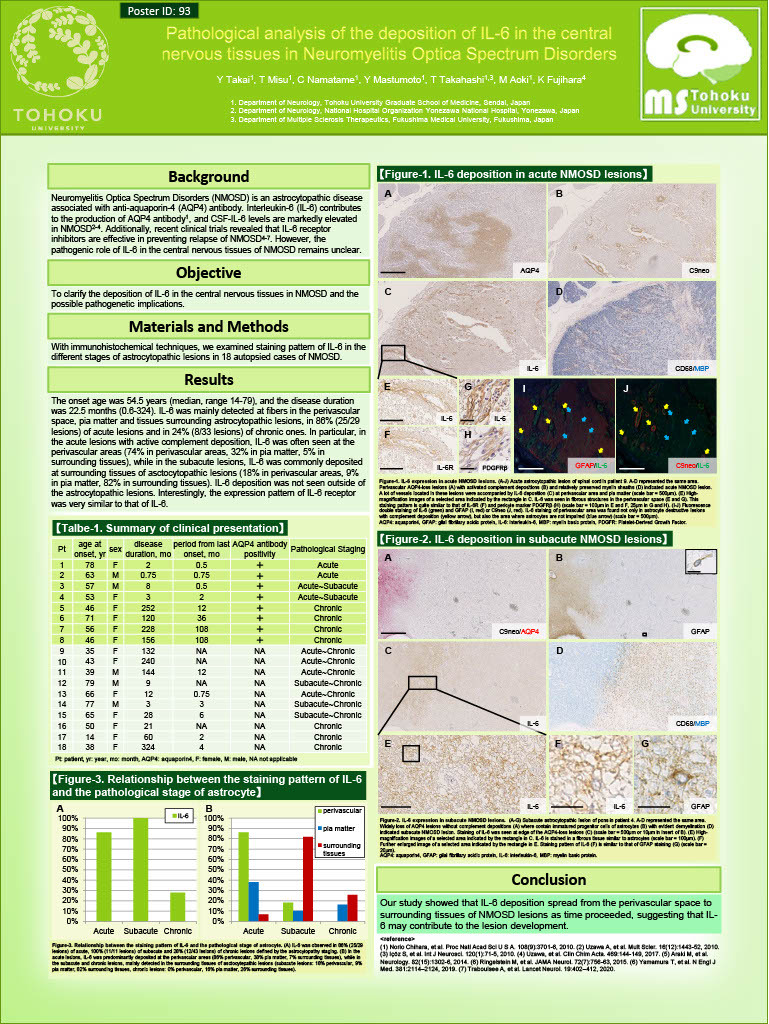
Neuromyelitis Optica Spectrum Disorders (NMOSD) is an astrocytopathic disease associated with anti-aquaporin-4 (AQP4) antibody. Interleukin-6 (IL-6) contributes to the production of AQP4 antibody, and CSF IL-6 levels are markedly elevated in NMOSD. Additonally, recent clinical trials revealed that IL-6 receptor inhibitors are effective in preventing relapse of NMOSD. However, the pethogenetic role of IL6 in the central nervous tissues of NMOSD remains unclear.
Objective:
To clarify the deposition of IL-6 in the central nervous tissues in NMOSD and the possible pathogenetic implications.
Methods:
With immunohistochemical techniques, we examined staining pattern of IL-6 in the different stages of astrocytopathic lesions in 18 autopsied cases of NMOSD.
Results:
The onset age was 54.5 years (median, range 14-79), and the disease duration was 22.5 months (0.6-324). IL-6 was mainly detected at fibers in the perivascular space, pia matter and tissues surrounding astrocytopathic lesions, in 86% (25/29 lesions) of acute lesions and in 24% (8/33 lesions) of chronic ones. In particular, in the acute lesions with active complement deposition, IL-6 was often seen at the perivascular areas (74% in perivascular areas, 32% in pia matter, 5% in surrounding tissues), while in the subacute lesions, IL-6 was commonly deposited at surrounding tissues of asctocytopathic lesions
(18% in perivascular areas, 9% in pia matter, 82% in surrounding tissues). IL-6 deposition was not seen outside of the astrocytopathic lesions. Interestingly, the expression pattern of IL-6 receptor was very similar to that of IL-6.
Conclusions:
Our study showed that IL-6 deposition spread from the perivascular space to surrounding tissues of NMOSD lesions as time proceeded, suggesting that IL-6 may contribute to the lesion development.